Angiotensin-converting enzyme 2
 From Wikipedia the free encyclopedia
From Wikipedia the free encyclopedia
Angiotensin-converting enzyme 2 (ACE2)[5] is an enzyme that can be found either attached to the membrane of cells (mACE2) in the intestines, kidney, testis, gallbladder, and heart or in a soluble form (sACE2).[6][7][8] Both membrane bound and soluble ACE2 are integral parts of the renin–angiotensin–aldosterone system (RAAS) that exists to keep the body's blood pressure in check. mACE2 is cleaved by the enzyme ADAM17 in a process regulated by substrate presentation. ADAM17 cleavage releases the extracellular domain creating soluble ACE2 (sACE2).[9] ACE2 enzyme activity opposes the classical arm of the RAAS by lowering blood pressure through catalyzing the hydrolysis of angiotensin II (a vasoconstrictor peptide which raises blood pressure) into angiotensin (1–7) (a vasodilator).[8][10][11] Angiotensin (1-7) in turns binds to MasR receptors creating localized vasodilation and hence decreasing blood pressure.[12] This decrease in blood pressure makes the entire process a promising drug target for treating cardiovascular diseases.[13][14]
mACE2 also serves as the entry point into cells for some coronaviruses, including HCoV-NL63, SARS-CoV, and SARS-CoV-2.[5] While mACE2's function is not that of a biological receptor, because of its receptor-like interaction with viruses it is also referred to as the ACE2 receptor.[15] The human version of the enzyme can be referred to as hACE2.[16]
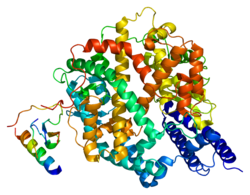
Structure
[edit]| Angiotensin-converting enzyme 2 | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Identifiers | |||||||||
| EC no. | 3.4.17.23 | ||||||||
| Databases | |||||||||
| IntEnz | IntEnz view | ||||||||
| BRENDA | BRENDA entry | ||||||||
| ExPASy | NiceZyme view | ||||||||
| KEGG | KEGG entry | ||||||||
| MetaCyc | metabolic pathway | ||||||||
| PRIAM | profile | ||||||||
| PDB structures | RCSB PDB PDBe PDBsum | ||||||||
| |||||||||
Membrane bound angiotensin-converting enzyme 2 (mACE2) is a zinc-containing metalloenzyme located on the surface of intestinal enterocytes, renal tubular cells and other cells.[6][17] mACE2 protein contains an N-terminal peptidase M2 domain and a C-terminal collectrin renal amino acid transporter domain.[17]
mACE2 is a single-pass type I membrane protein, with its enzymatically active domain exposed on the surface of cells in the intestines and other tissues.[6][7] The extracellular domain of mACE2 can be cleaved from the transmembrane domain by another enzyme known as ADAM17 a member of the sheddase enzyme family, during the protective phase of RAAS, the Renin–Angiotensin–Aldosterone System, which regulates our body's blood pressure. The resulting cleaved protein is known as soluble ACE2 or sACE2. It is released into the bloodstream where one of sACE2's functions is to turn excess angiotensin II into angiotensin 1-7 which binds to MasR receptors creating localized vasodilation and hence decreasing blood pressure. Excess sACE2 may ultimately be excreted in the urine.[18][19]
Location within the human body
[edit]mACE2 is attached to the cell membrane of mainly enterocytes of the small intestine and duodenum, proximal tubular cells of the kidneys, glandular cells of the gallbladder, as well as Sertoli cells and Leydig cells of the testis.[6] The expression profile of mACE2 in the human body was recently thoroughly evaluated by the Human Protein Atlas team using a large-scale multiomics approach combining several different methods for analysis of gene expression, including a stringent immunohistochemical analysis using two independent antibodies.[6][20] In addition to the above-mentioned issues, mACE2 expression was also seen in endothelial cells and pericytes of blood vessels within certain tissues, cardiomyocytes in heart tissue, and a smaller subset of cells within the thyroid gland, epididymis, seminal vesicle, pancreas, liver and placenta. Despite the fact that the respiratory system is the primary route of SARS-CoV-2 infection, very limited expression is seen, both at protein and mRNA level. The expression within the respiratory system is mainly restricted to the upper bronchial and nasal epithelia, especially in the ciliated cells.[21]
Function
[edit]As part of the renin–angiotensin–aldosterone system (RAAS) protective phase, soluble ACE2's (sACE2) important function is to act as a counterbalance to the angiotensin-converting enzyme (ACE). ACE cleaves angiotensin I hormone into the vasoconstricting angiotensin II which causes a cascade of hormonal reactions which is part of the body's harmful phase of RAAS, which ultimately leads to an increase in the body's blood pressure. ACE2 has an opposing effect to ACE, degrading angiotensin II into angiotensin (1-7), thereby lowering blood pressure.[22][23]
sACE2, as part of RAAS's protective phase, cleaves the carboxyl-terminal amino acid phenylalanine from angiotensin II (Asp-Arg-Val-Tyr-Ile-His-Pro-Phe) and hydrolyses it into the vasodilator angiotensin (1-7) (H-Asp-Arg-Val-Tyr-Ile-His-Pro-OH), which binds to Mas Receptors and ultimately leads to a decrease in blood pressure.[24][17] sACE2 can also cleave numerous peptides, including [des-Arg9]-bradykinin, apelin, neurotensin, dynorphin A, and ghrelin.[17]
mACE2 also regulates the membrane trafficking of the neutral amino acid transporter SLC6A19 and has been implicated in Hartnup's disease.[25][26][27]
Research in mice has shown that ACE2 (whether it is the membrane bound version or soluble is inconclusive) is involved in regulation of the blood glucose level but its mechanism is yet to be confirmed.[28][29]
Coronavirus entry point
[edit]As a transmembrane protein, mACE2 serves as the main entry point into cells for some coronaviruses, including HCoV-NL63,[5] SARS-CoV (the virus that causes SARS),[30][31][32] and SARS-CoV-2[33] (the virus that causes COVID-19).[34][35][36][37][38] More specifically, the binding of the spike S1 protein of SARS-CoV and SARS-CoV-2 to the enzymatic domain of mACE2 on the surface of cells results in endocytosis and translocation of both the virus and the enzyme into endosomes located within cells.[39][40] In culture blocking endocytosis traps the virus on the surface.[41] The SARS-CoV-2 spike protein itself is known to damage the endothelium via downregulation of ACE2.[42]
The receptor-binding domain (RBD) of spike protein, located on the virus’s surface, specifically attaches to human cell receptors.[38] ACE2 is essential as it’s a cell surface receptor that lets the virus get into and infect cells. The spike protein’s RBD of SARS-CoV-2 links to ACE2, enabling viral entry and reproduction within cells.[38] In addition the attachment of SP-A and SP-D residues to ACE2 could potentially diminish the strength of the interaction between the spike protein and ACE2.[38]
The binding of the SARS-CoV-2 virus through mACE2 receptors present in heart tissue may be responsible for direct viral injury leading to myocarditis. In a study done during the SARS outbreak, SARS virus RNA was ascertained in the autopsy of heart specimens in 35% of the patients who died due to SARS.[43] It was also observed that an already diseased heart has increased expression of mACE2 receptors contrasted to healthy individuals.[44] This entry process also requires priming of the S protein by the host serine protease TMPRSS2, the inhibition of which is under current investigation as a potential therapeutic.[45][21] It has also been shown that disruption of S-protein glycosylation significantly impairs viral entry, indicating the importance of glycan-protein interactions in the process.[46]
This has led some to hypothesize that decreasing the levels of mACE2, in cells, might help in fighting the infection. Furthermore, according to studies conducted on mice, the interaction of the spike protein of the coronavirus with mACE2 induces a drop in the levels of mACE2 in cells through internalization and degradation of the protein and hence may contribute to lung damage.[47][48]
On the other hand, sACE2 has been shown to have a protective effect against virus-induced lung injury by increasing the production of the vasodilator angiotensin 1–7.[47] Furthermore, some researchers have hypothesized that sACE2 (which is created during the Protective Phase of RAAS) is not only involved in binding to angiotensin II to create angiotensin I-7, which lowers blood pressure by vasodilation, but that free and soluble ACE2 may also be binding to coronavirus spike proteins, hence making those coronavirus spikes unavailable for binding to mACE-2 sites.[37] But even with only tiny amounts of mACE2, SARS-CoV-2 virus can gain entry into cells if TMPRSS2 is present.[49]
Both ACE inhibitors and angiotensin II receptor blockers (ARBs) that are used to treat high blood pressure have been shown in rodent studies to upregulate mACE2 expression, possibly affecting the severity of coronavirus infections.[50][51]
However, a systematic review and meta-analysis published on July 11, 2012, found that "use of ACE inhibitors was associated with a significant 34% reduction in risk of pneumonia compared with controls." Moreover, "the risk of pneumonia was also reduced in patients treated with ACE inhibitors who were at higher risk of pneumonia, in particular those with stroke and heart failure. Use of ACE inhibitors was also associated with a reduction in pneumonia related mortality, although the results were less robust than for overall risk of pneumonia."[52] An April 2020 study of patients hospitalized in Hubei Province in China found a death rate of 3.7% for patients with hypertension who were taking ACE inhibitors or ARBs. The death rate was compared with 9.8% of hospitalized patients with hypertension not taking such drugs, suggesting that ACE inhibitors and ARBs are not harmful and may help against the coronavirus.[53]
Despite lack of conclusive evidence, some have advocated for or against the cessation of ACE inhibitor or ARB treatment in COVID-19 patients with hypertension.[54] However, multiple professional societies and regulatory bodies have recommended continuing standard ACE inhibitor and ARB therapy.[55][56][57]
Plasma ACE2 levels predict outcome of COVID-19 in hospitalized patients, with higher plasma levels being correlated with worse disease outcomes. Patients with high blood pressure or heart disease show elevated ACE2 plasma levels.[58]
Given its role as the SARS-CoV-2 entry receptor, it has been repeatedly hypothesised that population variation in ACE2 may contribute to an individual's genetic susceptibility to COVID-19.[59][60] Several studies have reported that ACE2 missense variants can alter its binding affinity for the spike protein,[61][62][63] and consequently its susceptibility to SARS-CoV-2 pseudovirus entry,[64] and there is strong evidence of individuals who carry rare variants in ACE2 that could confer total resistance to SARS-CoV-2 infection.[63] The expression level of ACE2 at the cell surface is another critical factor affecting viral susceptibility and probably plays a role in the tissue tropism of the virus[64] and many suspected COVID-19 associated ACE2 variants affect expression.[60] In fact, SARS-CoV-2's viral tropism is dependent on ACE2 tissue distribution and expression.[65] For example, genetic variants placed in the X chromosome (rs190509934:C) have been related to lower expression levels of ACE2 enzyme. This would lead to an increased number of entries and infections performed by the SARS-CoV-2 virus. Moreover, those variants have shown a 37% reduction in expression of the protein and a remarkable protection from severe outcomes (respiratory failure and death).[66]
Recombinant human ACE2
[edit]Recombinant human ACE2 (rhACE2) is surmised to be a novel therapy for acute lung injury, and appeared to improve pulmonary blood flow and oxygen saturation in piglets with a lipopolysaccharide-induced acute respiratory distress syndrome.[67] The half-life of rhACE2 in human beings is about 10 hours, and the onset of action is 30 minutes in addition to the course of effect (duration) of 24 hours.[67] Several findings suggest that rhACE2 may be a promising drug for those with intolerance to classic renin–angiotensin system inhibitors (RAS inhibitors) or in diseases where circulating angiotensin II is elevated.[67]
An in vitro study focused on the early stages of infection found that clinical-grade human recombinant soluble ACE2 (hrsACE2) reduced SARS-CoV-2 recovery from vero cells by a factor of 1,000–5,000. The equivalent mouse rsACE2 did not have such an effect. This study suggests that rhsACE2 not only restores the renin-angiotensin system to balance as in the earlier ARDS studies, but also directly slows down infection by this virus – possibly as a decoy.[68] ACE2 mutants have been engineered with even higher affinity for SARS-CoV-2 Spike and shown to effectively neutralise the virus in vitro.[69] An ACE2 triple mutant that displayed nanomolar binding to Spike (sACE2.v2.4),[69] was later shown to block pseudovirus cell entry in human lung cell lines and prevent SARS-CoV-2 induced ARDS in an ACE2 humanized mouse model.[70]
Infused rhACE2 has been evaluated in clinical trials for the treatment of acute respiratory distress syndrome (ARDS).[71] rhACE2 is in phase II trial for severe COVID-19.[72]
See also
[edit]References
[edit]- ^ a b c GRCh38: Ensembl release 89: ENSG00000130234 – Ensembl, May 2017
- ^ a b c GRCm38: Ensembl release 89: ENSMUSG00000015405 – Ensembl, May 2017
- ^ "Human PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ "Mouse PubMed Reference:". National Center for Biotechnology Information, U.S. National Library of Medicine.
- ^ a b c "Gene: ACE2, angiotensin I converting enzyme 2". National Center for Biotechnology Information (NCBI). U.S. National Library of Medicine. 2020-02-28.
- ^ a b c d e Hikmet F, Méar L, Edvinsson Å, Micke P, Uhlén M, Lindskog C (July 2020). "The protein expression profile of ACE2 in human tissues". Molecular Systems Biology. 16 (7): e9610. doi:10.15252/msb.20209610. PMC 7383091. PMID 32715618.
- ^ a b Hamming I, Timens W, Bulthuis ML, Lely AT, Navis G, van Goor H (June 2004). "Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis". The Journal of Pathology. 203 (2): 631–637. doi:10.1002/path.1570. PMC 7167720. PMID 15141377.
- ^ a b Donoghue M, Hsieh F, Baronas E, Godbout K, Gosselin M, Stagliano N, et al. (September 2000). "A novel angiotensin-converting enzyme-related carboxypeptidase (ACE2) converts angiotensin I to angiotensin 1-9". Circulation Research. 87 (5): E1 – E9. doi:10.1161/01.RES.87.5.e1. PMID 10969042.
- ^ Lambert DW, Yarski M, Warner FJ, Thornhill P, Parkin ET, Smith AI, et al. (August 2005). "Tumor Necrosis Factor-α Convertase (ADAM17) Mediates Regulated Ectodomain Shedding of the Severe-acute Respiratory Syndrome-Coronavirus (SARS-CoV) Receptor, Angiotensin-converting Enzyme-2 (ACE2)". Journal of Biological Chemistry. 280 (34): 30113–30119. doi:10.1074/jbc.M505111200. PMC 8062222. PMID 15983030.
- ^ Keidar S, Kaplan M, Gamliel-Lazarovich A (February 2007). "ACE2 of the heart: From angiotensin I to angiotensin (1-7)". Cardiovascular Research. 73 (3): 463–469. doi:10.1016/j.cardiores.2006.09.006. PMID 17049503.
- ^ Wang W, McKinnie SM, Farhan M, Paul M, McDonald T, McLean B, et al. (August 2016). "Angiotensin-Converting Enzyme 2 Metabolizes and Partially Inactivates Pyr-Apelin-13 and Apelin-17: Physiological Effects in the Cardiovascular System". Hypertension. 68 (2): 365–377. doi:10.1161/HYPERTENSIONAHA.115.06892. PMID 27217402. S2CID 829514.
- ^ Chamsi-Pasha MA, Shao Z, Tang WH (March 2014). "Angiotensin-converting enzyme 2 as a therapeutic target for heart failure". Current Heart Failure Reports. 11 (1). Springer Science and Business Media LLC: 58–63. doi:10.1007/s11897-013-0178-0. PMC 3944399. PMID 24293035.
The discovery of ACE2 and its role in counteracting the effect of Ang-II through Ang(1-7) formation ... An imbalance in ACE2/Ang-(1–7) and ACE/Ang-II axes is critical in the development of cardiovascular diseases. The central role of ACE2, therefore, appears to counter ACE activity by reducing Ang-II bioavailability and increasing Ang(1-7) formation ... The use of RAS-modulating agents and molecules as novel therapeutic agents in hypertension and cardiovascular therapeutic research.
- ^ Chamsi-Pasha MA, Shao Z, Tang WH (March 2014). "Angiotensin-converting enzyme 2 as a therapeutic target for heart failure". Current Heart Failure Reports. 11 (1). Springer Science and Business Media LLC: 58–63. doi:10.1007/s11897-013-0178-0. PMC 3944399. PMID 24293035.
Studies with recombinant human ACE2 (rhACE2) have shown beneficial cardiac effects [18, 36]. rhACE2 has anti-fibrotic properties and can attenuate effect on systolic and diastolic dysfunction, presumably via Ang-II inhibition.
- ^ Mascolo A, Urbanek K, De Angelis A, Sessa M, Scavone C, Berrino L, et al. (March 2020). "Angiotensin II and angiotensin 1-7: which is their role in atrial fibrillation?". Heart Failure Reviews. 25 (2). Springer Science and Business Media LLC: 367–380. doi:10.1007/s10741-019-09837-7. PMID 31375968. S2CID 199388175.
the possibility of using the A1-7 or ACE2 analogues, to enlarge current therapeutic options for AF, may represent an important field of research.
- ^ Sriram K, Insel P, Loomba R. "What is the ACE2 receptor?". www.asbmb.org. Retrieved 2025-05-25.
- ^ Kasmi Y, Khataby K, Souiri A (2019). "Coronaviridae: 100,000 Years of Emergence and Reemergence". In Ennaji MM (ed.). Emerging and Reemerging Viral Pathogens: Fundamental and Basic Virology Aspects of Human, Animal and Plant Pathogens. Vol. 1. Elsevier. p. 135. ISBN 978-0-12-819400-3.
- ^ a b c d Turner AJ (2015). "Chapter 25: ACE2 Cell Biology, Regulation, and Physiological Functions". In Unger T, Ulrike M, Steckelings UM, dos Santos RA (eds.). The Protective Arm of the Renin Angiotensin System (RAS): Functional Aspects and Therapeutic Implications. Academic Press. pp. 185–189. doi:10.1016/B978-0-12-801364-9.00025-0. ISBN 978-0-12-801364-9. S2CID 88645177.
- ^ Lambert DW, Yarski M, Warner FJ, Thornhill P, Parkin ET, Smith AI, et al. (August 2005). "Tumor necrosis factor-alpha convertase (ADAM17) mediates regulated ectodomain shedding of the severe-acute respiratory syndrome-coronavirus (SARS-CoV) receptor, angiotensin-converting enzyme-2 (ACE2)". The Journal of Biological Chemistry. 280 (34): 30113–30119. doi:10.1074/jbc.M505111200. PMC 8062222. PMID 15983030.
- ^ Patel VB, Clarke N, Wang Z, Fan D, Parajuli N, Basu R, et al. (January 2014). "Angiotensin II induced proteolytic cleavage of myocardial ACE2 is mediated by TACE/ADAM-17: a positive feedback mechanism in the RAS". Journal of Molecular and Cellular Cardiology. 66: 167–176. doi:10.1016/j.yjmcc.2013.11.017. PMID 24332999.
- ^ The Human Protein Atlas. "ACE2 protein expression summary". www.proteinatlas.org. Retrieved 12 May 2021.
- ^ a b Jackson CB, Farzan M, Chen B, Choe H (January 2022). "Mechanisms of SARS-CoV-2 entry into cells". Nature Reviews. Molecular Cell Biology. 23 (1): 3–20. doi:10.1038/s41580-021-00418-x. PMC 8491763. PMID 34611326.
- ^ Hu Y, Liu L, Lu X (2021). "Regulation of Angiotensin-Converting Enzyme 2: A Potential Target to Prevent COVID-19?". Frontiers in Endocrinology. 12: 725967. doi:10.3389/fendo.2021.725967. PMC 8569797. PMID 34745001.
- ^ Singh B, Singh D, Verma V, Yadav R, Kumar R (December 2021). "Angiotensin-converting enzyme 2 as a potential therapeutic target for COVID-19: A review". Journal of Pharmaceutical Analysis. 12 (2): 215–220. doi:10.1016/j.jpha.2021.12.003. PMC 8677424. PMID 34934510.
- ^ Santos RA, Simoes e Silva AC, Maric C, Silva DM, Machado RP, de Buhr I, et al. (July 2003). "Angiotensin-(1-7) is an endogenous ligand for the G protein-coupled receptor Mas". Proceedings of the National Academy of Sciences of the United States of America. 100 (14): 8258–8263. Bibcode:2003PNAS..100.8258S. doi:10.1073/pnas.1432869100. PMC 166216. PMID 12829792.
- ^ Kowalczuk S, Bröer A, Tietze N, Vanslambrouck JM, Rasko JE, Bröer S (August 2008). "A protein complex in the brush-border membrane explains a Hartnup disorder allele". FASEB Journal. 22 (8): 2880–2887. doi:10.1096/fj.08-107300. PMID 18424768.
- ^ Fairweather SJ, Bröer A, Subramanian N, Tumer E, Cheng Q, Schmoll D, et al. (October 2015). "Molecular basis for the interaction of the mammalian amino acid transporters B0AT1 and B0AT3 with their ancillary protein collectrin". The Journal of Biological Chemistry. 290 (40): 24308–24325. doi:10.1074/jbc.M115.648519. PMC 4591816. PMID 26240152.
- ^ Yan R, Zhang Y, Li Y, Xia L, Guo Y, Zhou Q (March 2020). "Structural basis for the recognition of SARS-CoV-2 by full-length human ACE2". Science. 367 (6485): 1444–1448. Bibcode:2020Sci...367.1444Y. doi:10.1126/science.abb2762. PMC 7164635. PMID 32132184.
- ^ Niu MJ, Yang JK, Lin SS, Ji XJ, Guo LM (2008). "Loss of angiotensin-converting enzyme 2 leads to impaired glucose homeostasis in mice". Endocrine. 34 (1–3): 56–61. doi:10.1007/s12020-008-9110-x. PMID 18956256. S2CID 46331895.
- ^ Putnam K, Shoemaker R, Yiannikouris F, Cassis LA (March 2012). "The renin-angiotensin system: a target of and contributor to dyslipidemias, altered glucose homeostasis, and hypertension of the metabolic syndrome". American Journal of Physiology. Heart and Circulatory Physiology. 302 (6): H1219 – H1230. doi:10.1152/ajpheart.00796.2011. PMC 3311482. PMID 22227126.
- ^ Fehr AR, Perlman S (2015). "Coronaviruses: an overview of their replication and pathogenesis". Coronaviruses. Methods in Molecular Biology. Vol. 1282. Springer New York. pp. 1–23. doi:10.1007/978-1-4939-2438-7_1. ISBN 978-1-4939-2437-0. PMC 4369385. PMID 25720466.
Many α-coronaviruses utilize aminopeptidase N (APN) as their receptor, SARS-CoV and HCoV-NL63 use angiotensin-converting enzyme 2 (ACE2) as their receptor, MHV enters through CEACAM1, and the recently identified MERS-CoV binds to dipeptidyl-peptidase 4 (DPP4) to gain entry into human cells (See Table 1 for a list of known CoV receptors).
- ^ Li F (October 2013). "Receptor recognition and cross-species infections of SARS coronavirus". Antiviral Research. 100 (1): 246–254. doi:10.1016/j.antiviral.2013.08.014. PMC 3840050. PMID 23994189.
- ^ Kuba K, Imai Y, Rao S, Gao H, Guo F, Guan B, et al. (August 2005). "A crucial role of angiotensin converting enzyme 2 (ACE2) in SARS coronavirus-induced lung injury". Nature Medicine. 11 (8): 875–879. doi:10.1038/nm1267. PMC 7095783. PMID 16007097.
- ^ "What are the official names of the disease and the virus that causes it?". Q&A on coronaviruses. World Health Organization. Archived from the original on 5 March 2020. Retrieved 22 February 2020.
- ^ Zhou P, Yang XL, Wang XG, Hu B, Zhang L, Zhang W, et al. (March 2020). "A pneumonia outbreak associated with a new coronavirus of probable bat origin". Nature. 579 (7798): 270–273. Bibcode:2020Natur.579..270Z. doi:10.1038/s41586-020-2012-7. PMC 7095418. PMID 32015507.
- ^ Xu X, Chen P, Wang J, Feng J, Zhou H, Li X, et al. (March 2020). "Evolution of the novel coronavirus from the ongoing Wuhan outbreak and modeling of its spike protein for risk of human transmission". Science China Life Sciences. 63 (3): 457–460. doi:10.1007/s11427-020-1637-5. PMC 7089049. PMID 32009228.
- ^ Lewis R (2020-02-20). "COVID-19 Vaccine Will Close in on the Spikes". DNA Science Blog. Public Library of Science. Archived from the original on 2020-02-22. Retrieved 2020-02-22.
- ^ a b Zipeto D, Palmeira JD, Argañaraz GA, Argañaraz ER (2020). "ACE2/ADAM17/TMPRSS2 Interplay May Be the Main Risk Factor for COVID-19". Frontiers in Immunology. 11: 576745. doi:10.3389/fimmu.2020.576745. PMC 7575774. PMID 33117379.
- ^ a b c d Yousefbeigi S, Marsusi F (2023-11-20). "Structural insights into ACE2 interactions and immune activation of SARS-CoV-2 and its variants: an in-silico study". Journal of Biomolecular Structure and Dynamics: 1–14. doi:10.1080/07391102.2023.2283158. ISSN 0739-1102.
- ^ Wang H, Yang P, Liu K, Guo F, Zhang Y, Zhang G, et al. (February 2008). "SARS coronavirus entry into host cells through a novel clathrin- and caveolae-independent endocytic pathway". Cell Research. 18 (2): 290–301. doi:10.1038/cr.2008.15. PMC 7091891. PMID 18227861.
- ^ Millet JK, Whittaker GR (April 2018). "Physiological and molecular triggers for SARS-CoV membrane fusion and entry into host cells". Virology. 517: 3–8. doi:10.1016/j.virol.2017.12.015. PMC 7112017. PMID 29275820.
- ^ Hansen SB, Yuan Z (March 2023). "Getting in on the action: New tools to see SARS-CoV-2 infect a cell". Cell Chemical Biology. 30 (3): 233–234. doi:10.1016/j.chembiol.2023.02.010. PMC 10018748. PMID 36931249. S2CID 257580098.
- ^ Lei Y, Zhang J, Schiavon CR, He M, Chen L, Shen H, et al. (April 2021). "SARS-CoV-2 Spike Protein Impairs Endothelial Function via Downregulation of ACE 2". Circulation Research. 128 (9): 1323–1326. doi:10.1161/CIRCRESAHA.121.318902. PMC 8091897. PMID 33784827.
- ^ Oudit GY, Kassiri Z, Jiang C, Liu PP, Poutanen SM, Penninger JM, et al. (July 2009). "SARS-coronavirus modulation of myocardial ACE2 expression and inflammation in patients with SARS". European Journal of Clinical Investigation. 39 (7): 618–625. doi:10.1111/j.1365-2362.2009.02153.x. PMC 7163766. PMID 19453650.
- ^ Rathore SS, Rojas GA, Sondhi M, Pothuru S, Pydi R, Kancherla N, et al. (November 2021). "Myocarditis associated with Covid-19 disease: A systematic review of published case reports and case series". International Journal of Clinical Practice. 75 (11): e14470. doi:10.1111/ijcp.14470. PMID 34235815. S2CID 235768792.
- ^ Akhmerov A, Marbán E (May 2020). "COVID-19 and the Heart". Circulation Research. 126 (10): 1443–1455. doi:10.1161/CIRCRESAHA.120.317055. PMC 7188058. PMID 32252591.
- ^ Novokmet M, Baković MP, Lauc G (1 April 2020). "Understanding Glycans in COVID-19 Drug Design". Genetic Engineering and Biotechnology News. Retrieved 2020-05-18.
- ^ a b Imai Y, Kuba K, Penninger JM (May 2008). "The discovery of angiotensin-converting enzyme 2 and its role in acute lung injury in mice". Experimental Physiology. 93 (5): 543–548. doi:10.1113/expphysiol.2007.040048. PMC 7197898. PMID 18448662.
- ^ Jia H (September 2016). "Pulmonary Angiotensin-Converting Enzyme 2 (ACE2) and Inflammatory Lung Disease". Shock. 46 (3): 239–248. doi:10.1097/SHK.0000000000000633. PMID 27082314. S2CID 3639219.
Once SARS-CoV binds to its receptor, the abundance on the cell surface, mRNA expression and the enzymatic activity of ACE2 are significantly reduced. ... These effects are, in part, due to enhanced shedding/internalizing processes. ... The spike protein binds to ACE2 and subsequently down regulated ACE2 protein expression and resulted in worsened acid aspiration pneumonia
- ^ Harrison AG, Lin T, Wang P (December 2020). "Mechanisms of SARS-CoV-2 Transmission and Pathogenesis". Trends in Immunology. 41 (12): 1100–1115. doi:10.1016/j.it.2020.10.004. PMC 7556779. PMID 33132005.
- ^ Nicholls J, Peiris M (August 2005). "Good ACE, bad ACE do battle in lung injury, SARS". Nature Medicine. 11 (8): 821–822. doi:10.1038/nm0805-821. PMC 7095949. PMID 16079870.
- ^ Diaz JH (May 2020). "Hypothesis: angiotensin-converting enzyme inhibitors and angiotensin receptor blockers may increase the risk of severe COVID-19". Journal of Travel Medicine. 27 (3). doi:10.1093/jtm/taaa041. PMC 7184445. PMID 32186711.
- ^ Caldeira D, Alarcão J, Vaz-Carneiro A, Costa J (July 2012). "Risk of pneumonia associated with use of angiotensin converting enzyme inhibitors and angiotensin receptor blockers: systematic review and meta-analysis". BMJ. 345 (jul11 1): e4260. doi:10.1136/bmj.e4260. PMC 3394697. PMID 22786934.
Our results suggest an important role of ACE inhibitors, but not ARBs, in reducing the risk of pneumonia. These data may discourage the withdrawal of ACE inhibitors in some patients with tolerable adverse events (namely, cough) who are at particularly high risk of pneumonia. ACE inhibitors also lowered the risk of pneumonia related mortality, mainly in patients with established disease, but the robustness of the evidence was weaker.
- ^ Zhang P, Zhu L, Cai J, Lei F, Qin JJ, Xie J, et al. (June 2020). "Association of Inpatient Use of Angiotensin-Converting Enzyme Inhibitors and Angiotensin II Receptor Blockers With Mortality Among Patients With Hypertension Hospitalized With COVID-19". Circulation Research. 126 (12): 1671–1681. doi:10.1161/CIRCRESAHA.120.317134. PMC 7265882. PMID 32302265.
- ^ Patel AB, Verma A (May 2020). "COVID-19 and Angiotensin-Converting Enzyme Inhibitors and Angiotensin Receptor Blockers: What Is the Evidence?". JAMA. 323 (18): 1769–1770. doi:10.1001/jama.2020.4812. PMID 32208485.
- ^ "Position Statement of the ESC Council on Hypertension on ACE-Inhibitors and Angiotensin Receptor Blockers". European Society of Cardiology (ESC). 13 March 2020.
- ^ "EMA advises continued use of medicines for hypertension, heart or kidney disease during COVID-19 pandemic". European Medicines Agency (EMA). 27 March 2020.
- ^ "HFSA/ACC/AHA Statement Addresses Concerns Re: Using RAAS Antagonists in COVID-19". American College of Cardiology (ACC). 27 March 2020.
- ^ Kragstrup TW, Singh HS, Grundberg I, Nielsen AL, Rivellese F, Mehta A, et al. (2021). "Plasma ACE2 predicts outcome of COVID-19 in hospitalized patients". PLOS ONE. 16 (6): e0252799. Bibcode:2021PLoSO..1652799K. doi:10.1371/journal.pone.0252799. PMC 8177449. PMID 34086837.
- ^ Cao Y, Li L, Feng Z, Wan S, Huang P, Sun X, et al. (2020-02-24). "Comparative genetic analysis of the novel coronavirus (2019-nCoV/SARS-CoV-2) receptor ACE2 in different populations". Cell Discovery. 6 (1): 11. doi:10.1038/s41421-020-0147-1. PMC 7040011. PMID 32133153.
- ^ a b Li J, Wang Y, Liu Y, Zhang Z, Zhai Y, Dai Y, et al. (February 2022). "Polymorphisms and mutations of ACE2 and TMPRSS2 genes are associated with COVID-19: a systematic review". European Journal of Medical Research. 27 (1): 26. doi:10.1186/s40001-022-00647-6. PMC 8861605. PMID 35193695.
- ^ Suryamohan K, Diwanji D, Stawiski EW, Gupta R, Miersch S, Liu J, et al. (April 2021). "Human ACE2 receptor polymorphisms and altered susceptibility to SARS-CoV-2". Communications Biology. 4 (1): 475. doi:10.1038/s42003-021-02030-3. PMC 8041869. PMID 33846513.
- ^ Santos TM, Lisboa AB, Rodrigues W, Gomes H, Abrahão J, Del-Bem LE (February 2022). "Human variation in the protein receptor ACE2 affects its binding affinity to SARS-CoV-2 in a variant-dependent manner". Journal of Biomolecular Structure & Dynamics. 41 (7): 2947–2955. doi:10.1080/07391102.2022.2042387. PMID 35196964. S2CID 247083671.
- ^ a b MacGowan SA, Barton MI, Kutuzov M, Dushek O, van der Merwe PA, Barton GJ (March 2022). "Missense variants in human ACE2 strongly affect binding to SARS-CoV-2 Spike providing a mechanism for ACE2 mediated genetic risk in Covid-19: A case study in affinity predictions of interface variants". PLOS Computational Biology. 18 (3): e1009922. Bibcode:2022PLSCB..18E9922M. doi:10.1371/journal.pcbi.1009922. PMC 8920257. PMID 35235558.
- ^ a b Shukla N, Roelle SM, Suzart VG, Bruchez AM, Matreyek KA (July 2021). "Mutants of human ACE2 differentially promote SARS-CoV and SARS-CoV-2 spike mediated infection". PLOS Pathogens. 17 (7): e1009715. doi:10.1371/journal.ppat.1009715. PMC 8284657. PMID 34270613.
- ^ Oudit GY, Wang K, Viveiros A, Kellner MJ, Penninger JM (March 2023). "Angiotensin-converting enzyme 2-at the heart of the COVID-19 pandemic". Cell. 186 (5): 906–922. doi:10.1016/j.cell.2023.01.039. PMC 9892333. PMID 36787743. S2CID 256460314.
- ^ Niemi ME, Daly MJ, Ganna A (September 2022). "The human genetic epidemiology of COVID-19". Nature Reviews. Genetics. 23 (9): 533–546. doi:10.1038/s41576-022-00478-5. PMC 9060414. PMID 35501396.
- ^ a b c Colafella KM, Uijl E, Danser J (2019). "Interference With the Renin–Angiotensin System (RAS): Classical Inhibitors and Novel Approaches". Encyclopedia of Endocrine Diseases. Elsevier. pp. 523–530. doi:10.1016/b978-0-12-801238-3.65341-2. ISBN 978-0-12-812200-6. S2CID 86384280.
- ^ Monteil V, Kwon H, Prado P, Hagelkrüys A, Wimmer RA, Stahl M, et al. (May 2020). "Inhibition of SARS-CoV-2 Infections in Engineered Human Tissues Using Clinical-Grade Soluble Human ACE2". Cell. 181 (4): 905–913.e7. doi:10.1016/j.cell.2020.04.004. PMC 7181998. PMID 32333836.
- ^ a b Chan KK, Dorosky D, Sharma P, Abbasi SA, Dye JM, Kranz DM, et al. (September 2020). "Engineering human ACE2 to optimize binding to the spike protein of SARS coronavirus 2". Science. 369 (6508): 1261–1265. Bibcode:2020Sci...369.1261C. doi:10.1126/science.abc0870. PMC 7574912. PMID 32753553.
- ^ Zhang L, Dutta S, Xiong S, Chan M, Chan KK, Fan TM, et al. (March 2022). "Engineered ACE2 decoy mitigates lung injury and death induced by SARS-CoV-2 variants". Nature Chemical Biology. 18 (3): 342–351. doi:10.1038/s41589-021-00965-6. PMC 8885411. PMID 35046611.
- ^ Khan A, Benthin C, Zeno B, Albertson TE, Boyd J, Christie JD, et al. (September 2017). "A pilot clinical trial of recombinant human angiotensin-converting enzyme 2 in acute respiratory distress syndrome". Critical Care. 21 (1): 234. doi:10.1186/s13054-017-1823-x. PMC 5588692. PMID 28877748.
- ^ "Apeiron Biologics moves forward with APN01 for treatment of COVID-19". www.thepharmaletter.com. Retrieved 3 April 2020.
External links
[edit]- Human ACE2 genome location and ACE2 gene details page in the UCSC Genome Browser.
- Angiotensin-converting enzyme 2 in Membranome database
- 3D structure of complex of a neurotransmitter sodium symporter B(0)AT1, ACE2, and SARS-CoV-2 receptor-binding domain in OPM database
- Overview of all the structural information available in the PDB for UniProt: Q9BYF1 (Angiotensin-converting enzyme 2) at the PDBe-KB.